Presacral Tumors
The presacral space is the area between the rectum and lowest part of your the spine, which is called the sacrum. The presacral space is inside the pelvis, behind the rectum and in front of the coccyx and sacrum. Normally it is empty, or it contains a pocket of fat.
Incidence
A tumor in this area is rare and can be benign or malignant (cancer). The presacral space may contain one of several kinds. The most common is sacrococcygeal teratoma. Others are retrorectal hamartoma (tailgut cyst), schwannoma, ganglioneuroma, and ependymoma. The outcomes for patients with benign presacral tumors are favorable.
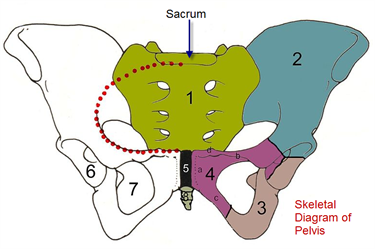
Diagram of Pelvis including Sacrum.The presacral space is inside the pelvis, behind the rectum and in front of the coccyx and sacrum. Source: Creative Commons License from Wikimedia Commons
Causes
A presacral tumor may be caused by:
- Congenital conditions present from birth
- Hereditary disorders such as Currarino syndrome
- Cancer that has metastized from another site in the body
Symptoms
Symptoms are often non-specific (are often found in many other diseases and conditions) making presacral tumors difficult to diagnose. In addition there may be no symptoms.
Some symptoms that associated with presacral tumors include:
- Pain in the lower back or rectal/pelvic area
- A feeling of heaviness
- Constipation
- Overflow incontinence
- Weight loss
Diagnosis
Physical exam and history: An exam of the body to check general signs of health, including checking for signs of disease, or anything else that seems unusual. Tests include:
- X-rays: An x-ray is a type of energy beam that can go through the body onto film, making pictures of areas inside the body.
- Laboratory tests: Medical procedures that test samples of tissue, blood, urine, or other substances in the body. These tests help to diagnose disease, plan and check treatment, or monitor the disease over time.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside of the body, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI).
Treatment
Surgery
Surgery is the mainstay of treatment for presacral tumors and is often also used to establish the diagnosis. The type of surgery in this area is called pelvic excision (removing the tumor) or pelvic resection.
Because of its rarity, few surgeons have experience in treating these complex lesions. Surgeons at large medical centers who perform a high volume of complex colorectal surgeries are more likely to have seen these tumors. At these centers, surgeons are supported by an experienced, multidisciplinary team.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are two types of radiation therapy. External radiation therapy uses a machine outside the body to send radiation toward the cancer. Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer. The way the radiation therapy is given depends on the type and stage of the cancer being treated.
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body ( systemic chemotherapy). When chemotherapy is placed directly into the spinal column, an organ, or a body cavity such as the abdomen, the drugs mainly affect cancer cells in those areas ( regional chemotherapy). The way the chemotherapy is given depends on the type and stage of the cancer being treated.
Prognosis
There have been significant improvements in the long-term outlook for patients with malignant presacral tumors. The continued development of adjuvant (after surgery) therapies are likely to further improve the outcomes further for malignant presacral tumors such as chordomas and sarcomas.


